The
Washington Post’s “Wonkblog” reviewed
a report by economists discussing “The stunning — and expanding — gap in life
expectancy between the rich and the poor”
(Max Ehrenfreund, Sept 18, 2015). One focus of the article, which is based on a
report from the National Academy of Sciences,
is that (in the words of the alternative title of the Wonkblog piece that
displays in the URL), “the government is spending more to help rich seniors
than poor ones”. A big reason for this is that the greater life expectancy of
the more well-to-do means that they collect benefits from Social Security and
Medicare for longer. But, of course, the real issue is that there is such a
difference in the life expectancy of rich and poor. Ehrenfreund illustrates
this with two dramatic graphs:

This is a pretty significant difference. What are
the reasons for it? The report (and the article based on it) indicate that
while differences in “lifestyle” (smoking and obesity, mainly) account for some
of the difference, it is less than 1/3. The study also alludes to the impact of
“stress”. This may seem vague, non-specific, or ubiquitous: aren’t we all stressed?
Don’t rich people have a lot of stress because wealth is often accompanied by
great responsibility? Such interpretations sometimes leads "stress" as a factor in longevity to be discounted by many
commentators. But the impact of stress on health is a real thing, and it is well
documented. Many people are familiar with the old terms “Type A” and “Type B” personalities,
and how being Type A (more stressed) can lead to a greater risk of disease,
particularly heart attack. But the real concern is a kind of stress that is
more common in poorer people. This is the continuous
stress, from worrying about whether you and your family will have enough food
to eat and a place to live, whether you will have a job, whether it is safe to
walk down the street, whether (especially if you are a young Black man) the
police are going to stop you at any moment, that has major negative health
effects. The mechanisms through which this occurs are incompletely elucidated,
but certainly involve the neuroendocrine system, the release of hormones that
prepare the body for “fight or flight” by refocusing blood flow to muscles,
increasing heart rate, etc. Such a response is very useful in an emergency, but when
it is happening most or all of the time, and the body does not have the time and
rest to fully recuperate, it results in real health damage. This hormonal
response allows a person to run fast, from an attacker or for sport, for a
short time, but if the challenge never stops, the body eventually wears out
This sort of stress on the body may be the “final
common pathway” through which many of the negative life situations that poorer
people are more likely to find themselves in exact their toll, but
there are also other factors. People’s health, and thus their life expectancy,
is to a large extent determined by their early childhood experience. The
relative income of their families of origin that affects their childhood nutrition
and education, their warmth in the winter, and the amount of transmitted stress
that their parents felt, is also a big determinant. While this disparity at the
start of life is something that can be mitigated, by some, through future success,
it can never be completely erased. That is, while rich people from poor
backgrounds may have better health later in life than those who stay poorer,
they have on average worse health than those who started out wealthy and stayed
that way. “Choose your parents wisely,”
I tell my medical students, “if they are
both long-lived and rich, it bodes well for your future health.” Luckily
for them, the majority of medical students come from at least
upper-middle-income families.
Another big determinant is education, and many
studies show the correlation of higher levels of education with longer life and
better health. Of course, education is highly correlated with income, both on
the front end (children from higher-income families are more likely to achieve
higher educational levels) and on the back end (those children from families of
lower socioeconomic status who are successful have usually become so through
education). In the US, income is related to education in part because our
schools are largely funded by local tax bases, so that wealthier people live in
better funded, and educationally better, school districts. People from other
countries often have difficulty understanding that we have “good” and “bad” school
districts; as one friend said “where I come from all schools are the same! No
one would choose where to live based on the quality of the schools!” This
concept is so alien to me that I had
difficulty understanding them!
 In addition, education does not take place only in
school. Children from upper-income families are more likely to have educated
parents, who not only encourage them to pursue educational success, but read to
them and talk to them from the very beginning of their lives. These are also
families in which survival needs do not displace the priority of children
getting an education. In 1943, the psychologist Abraham Maslow published his
hierarchy of needs; survival must come before self-actualization. This was
originally conceived of for the individual, but is also true of families and
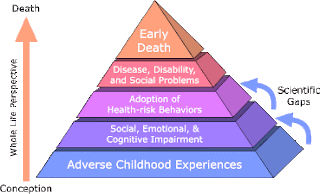
communities. A similar pyramid has been developed to describe the impact of Adverse
Childhood Events (ACEs). ACEs are a ways of thinking about the combination of
negative impacts including hunger, homelessness, physical abuse, sexual abuse,
neighborhood dangerousness, etc., that have been shown to have a lifelong negative
impact. In addition to being associated with higher future rates of drug abuse
and mental illness, they are associated with higher rates of just about everything bad.
The Adverse Childhood Experiences study
conducted by Kaiser Permanente beginning in 1995-97 is the most significant
study on this topic. It is ongoing and being replicated in many other
countries.
In addition, education does not take place only in
school. Children from upper-income families are more likely to have educated
parents, who not only encourage them to pursue educational success, but read to
them and talk to them from the very beginning of their lives. These are also
families in which survival needs do not displace the priority of children
getting an education. In 1943, the psychologist Abraham Maslow published his
hierarchy of needs; survival must come before self-actualization. This was
originally conceived of for the individual, but is also true of families and
communities. A similar pyramid has been developed to describe the impact of Adverse
Childhood Events (ACEs). ACEs are a ways of thinking about the combination of
negative impacts including hunger, homelessness, physical abuse, sexual abuse,
neighborhood dangerousness, etc., that have been shown to have a lifelong negative
impact. In addition to being associated with higher future rates of drug abuse
and mental illness, they are associated with higher rates of just about everything bad.
The Adverse Childhood Experiences study
conducted by Kaiser Permanente beginning in 1995-97 is the most significant
study on this topic. It is ongoing and being replicated in many other
countries.
Of course, lower income people are exposed to other risks beyond
these. People living in “worse” neighborhoods have a greater likelihood of
being homicide victims. Those neighborhoods are much more likely to be exposed
to environmental pollutants in the air and water and even from the earth (such
as toxic waste dumps). Many lower-income people work in more dangerous jobs, especially true in rural areas (farming, ranching, logging, highway
construction, etc.) Indeed, the potential for “confounding” results from such
exposures was the reason that Michael Marmot and his colleagues did their
classic series of studies showing the direct correlation of higher
socioeconomic status (class) and better health by examining people who worked
for the government in the same offices in London (thus the name “the Whitehall studies”).
 Wealthy people have a longer life expectancy than poor
people, and wealthy
countries have longer life expectancies than poorer
countries, and those with wider gaps between the rich and poor have wider gaps
in life expectancy; in this regard the US is at greater risk than wealthy
nations with smaller gaps. The neat
interactive website from Gapminder allows you
to track wealth with life expectancy over time since 1800. The GINI index measures
the income disparities within countries, and its use allows correlating income
inequality with life expectancy; like several other health measures (e.g.,
infant mortality) life expectancy goes down with increasing inequality even
when a country (such as the US) is rich overall.
Wealthy people have a longer life expectancy than poor
people, and wealthy
countries have longer life expectancies than poorer
countries, and those with wider gaps between the rich and poor have wider gaps
in life expectancy; in this regard the US is at greater risk than wealthy
nations with smaller gaps. The neat
interactive website from Gapminder allows you
to track wealth with life expectancy over time since 1800. The GINI index measures
the income disparities within countries, and its use allows correlating income
inequality with life expectancy; like several other health measures (e.g.,
infant mortality) life expectancy goes down with increasing inequality even
when a country (such as the US) is rich overall.
So yes, our Social Security and Medicare systems
mean that those who live longer will have more financial benefit, and that they
are more likely to be more well-to-do than those who die younger. In addition,
those who are poorer are more likely to live longer with disability. But the
real news is that poverty and social deprivation work in many synergistic ways
to decrease the health of the poor. This is what we need a coordinated and
comprehensive strategy to address.